
We’ve all heard the expressions, “It takes two to tango” and “Two heads are better than one.” The world has made it pretty clear that when given the choice of one or two, it’s best to go with two. However, in the world of health insurance, this logic doesn’t quite stand up.
When your employees are signing up for your company health insurance, they may ask you if it’s okay to have two separate health insurance policies. You also might be wondering if you should enroll in two health care plans yourself. Confused? Don’t be.
In this article, we explain what happens when you have primary and secondary coverage. This can help your employees decide if having two sets of monthly premiums are worth the cost and benefits for potential medical expenses.
Here are eight common FAQs for this topic, so you won’t have to do a double-take when someone asks you about double coverage.
Why would someone have more than one health insurance plan?
Allow us to explain a thing (or two). Usually people wonder about multiple health coverage because they’re insured under a spouse’s plan, a Medicare plan, a parent’s plan (if they’re under 26), or have a child who is already covered. Seventy-eight percent of American employers—both large and small—currently offer health insurance. With so many people getting coverage at work, the dual plan question is bound to come up at some point.
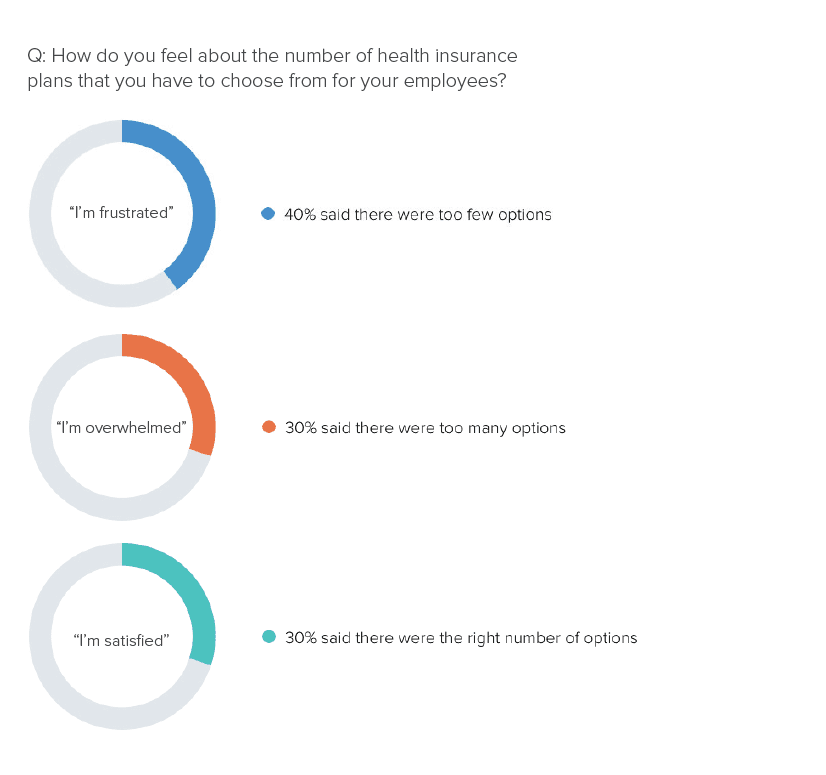
People also crave options. A Gusto report on the state of health benefits for small businesses found that only a third of employers feel good about the number of plans they had to pick from. That dissatisfaction is not just relegated to employers—employees also want more choices.
How do multiple health insurance plans work?
Having two health insurance policies isn’t like life insurance, where having a secondary insurance plan could be beneficial. Unfortunately, enrolling in two health plans doesn’t double your options when it comes to medical coverage. It can actually act more like a double negative because your two insurance companies will have to duke it out over who is going to pay for your medical bills. One of them will eventually pay, but you may not have a say as to which one that is.
When there are two health insurance plans, which one pays?
If you have dual coverage, health insurance companies will determine which of them are the primary and secondary payers through a process called coordination of benefits, or COB. This helps carriers and participants get on the same page when there are two types of insurance plans. It enables people to receive full coverage for their medical bills, while preventing carriers from overpaying on medical claims by accidentally sending you or your doctors double the reimbursement.
What is the difference between primary insurance and secondary coverage?
A COB assigns one plan as the main form of insurance, and the other as the secondary health insurance. The primary coverage picks up the tab on most of the benefits, and the secondary plan takes care of the benefits that the other plan didn’t cover. In the end, a person with dual coverage can sometimes pay nearly nothing after their deductibles are met—however this happens on a case-by-case basis, so remaining cost-sharing or out-of-pocket expenses, such as copayments and coinsurance, could still remain as part of your total medical costs. Even with a good COB in place, you still have to select medical plans that suit your needs, lining up coverage options as best as possibile, and be ready to deal with a gigantic pile of paperwork for the health care services you require.
Pro tip: Make sure your team always keeps their COB up to date. This stuff is complicated, so any error can send not one, but two carriers into a tailspin.
What are the pros and cons of double health coverage?
The downsides of two health insurances:
Employees will end up paying twice for health insurance coverage.
Most of the time, coverage is redundant—you can’t pick and choose what you want.
It can be an administrative mess, especially when claims are involved. Employees have to handle all the claims on their own, and things can get complicated if one plan is an HMO and the other is a PPO.
The upsides of two health insurances:
If one plan doesn’t have in-depth coverage, the other can fill in the gaps for health care costs. For example, if the primary health care plan pays 80 percent of a procedure, the other plan could handle the difference.
If you’re going to meet the deductible on both plans, it may help you get more out of your coverage.
Can employees benefit from having two health care plans?
For most people, double coverage is double trouble. The price tag and pyramid of paperwork can make it too complicated to be truly useful. Instead, your team should aim to pick a single plan that offers the best coverage for their needs. Keep in mind that you shouldn’t weigh in on your employees’ choices. If you have a broker, they can help dispel the myth that enrolling in two medical policies is better than one.
What is another type of coverage that would be considered secondary?
A second medical insurance isn’t the only example of secondary coverage. The latter can also consist of separate plans that include accident insurance, supplemental hospital care, medicare coverage, as well as disability, vision, and dental plans.
My employee has two health insurance plans. How do they know which one is the main one?
There are a few basic rules, depending on their situation. Here are the most common scenarios:
For your employee
Their company-sponsored plan covers them first (if it’s a group employer’s plan with 20 or more people enrolled).
Their spouse’s plan covers them after that.
If both your employee and their spouse are covered twice, the spouse’s employer coverage is the main one, and theirs is the secondary coverage.
For their kids
If both parents’ health plans include their child as a dependent, such as in instances of joint custody for children of divorced or separated parents, the birthday rule gets celebrated (or put into effect). It might sound a bit wacky, but here goes:
The parent who has a birthday earlier in the calendar year is the one whose plan gets chosen as the primary.
Do both parents have the same birthday? Then the health insurance that is oldest will be the primary payer.
If an employee’s child is under 26, employed, and covered as a dependent on their parent’s plan, then the child’s workplace plan is the primary one. With few exceptions, grown-up kids who are older than 26 can’t be covered under their parents’ plans.
For Medicare enrollees
Things get a bit more complicated when Medicare comes into the picture. Generally, if your employee has a group health plan in addition to Medicare, the group plan is the first in line. However, if that plan is designed for retirees, then Medicare will be the primary plan.
Chart: quick guide on dual coverage
Scenario | Primary Insurance | Secondary Insurance |
|---|---|---|
Married employees | Your employer | Spouse’s employer |
Employees’ children | Parent with first birthday during calendar year | Parent with later birthday during calendar year |
Employee’s employed dependents under 26 years | Dependent’s employer | Parent’s employer |
Employee’s dependents under 26 years on college health plan | School-sponsored plan | Parent’s plan |
Medicare enrollees | Employer’s group plan | Medicare |
Retired Medicare enrollees | Medicare | Group plan |



