
When an employee waives health coverage, there are a handful of rules you’ll need to follow to keep things flowing smoothly.
In this article, we’ll explain how to waive coverage for your employee, all while keeping everyone’s uncertainty at bay.
Why do people decline employer-sponsored health insurance?
There are a few main reasons your employees may reject the health coverage you’re offering:
They’re already under a family member’s plan.
They’re receiving insurance from another employer.
They prefer an individual health plan because it offers better benefits or is more affordable.
How do employees waive health coverage?
1. Know the basics.
The Affordable Care Act used to require everyone to sign up for a health plan, get an exemption, or wind up with a fine from the IRS. Starting in 2019, that fee no longer applies.
However, having health insurance can help protect your employees’ health and financial wellbeing and give them peace of mind. You may also want to warn them that opting out of insurance at work means their family won’t be eligible for that plan either.
2. Know the timeline.
Employees can only decline employer-sponsored insurance during an open enrollment period, which they may be in the middle of if they just started at your company. Otherwise, they’ll have to wait for the next enrollment period to come around, unless they have a qualifying life event, like a birth or marriage.
If they ever lose their other source of coverage, they’ll be able to jump back on your plan immediately. Keep in mind that this only applies if their coverage has expired or otherwise ended—not from them stopping payment or deciding they don’t want it anymore.
3. Help them assess their options.
If an employee is interested in waiving, give them a copy of the summary of benefits and coverage so they can compare it with other options they’re interested in or already have in place through a partner, a parent if they’re under 26 (yay ACA!), the individual market, or another source.
You should also let them know that if the option you’re providing meets the ACA standards and they waive, they no longer qualify for any premium marketplace subsidies. It may look like they qualify at first, but the IRS will see that you offered it and will take back any credit they received.
4. Obtain their waiver of coverage.
Now, have them fill out a waiver of coverage form, which you can get from your carrier. They’ll have to fill out the following details:
Name
Social Security number
Policy number and carrier information for their main plan
Waiver of coverage explanation
The waiver of coverage explanation typically contains language that says they understand that if they reject coverage, they won’t be able to join the plan until the next open enrollment period, or if they experience a qualifying life event. It also lays out what those special periods entail.
Here’s a sample form from Anthem to give you an idea of what they’ll be dealing with.
5. That’s it!
Your employee has successfully waived coverage the right way.
What should I do if my employees want to waive health coverage?
1. Brush up on your responsibilities.
As an employer, your goal is to make sure all full-time employees have the chance to sign up for health insurance during open enrollment. Everything rides on this.
If someone wasn’t given an opportunity, they can sign up for a plan from HealthCare.gov and then claim a premium subsidy on their taxes. This can trigger an audit for any employer, and if you’re a company with 50 or more FTEs, you may need to pay a penalty. Basically, it tells the IRS that you didn’t offer your employees adequate health insurance, even though you were supposed to.
2. Know your carrier’s participation requirements.
Most insurance companies require a certain percentage of employees to join a group plan. The number is usually around 75 percent, but it varies by carrier.
Don’t worry: If an employee has a valid reason for declining coverage, like they have existing coverage with their spouse’s employer, the carrier won’t apply that person toward your minimum. However, if they don’t have a valid reason, it’ll affect the participation calculation for your plan.
Keep in mind that if you’re contributing 100% toward your employees’ health plans and your carrier stipulates that you must have 100% enrollment on the plan, your employees may not be able to decline your plan.
3. Educate, educate, educate.
Before any decisions are made, make sure you’ve properly educated the team on what their choices are.
Not only is this important for their well-being, but it can also have potential repercussions if you have more than 50 FTEs and they enroll in another option and then claim a premium subsidy.
If an employee buys a plan that doesn’t meet the minimum value standard, it’s not ideal, but everything won’t come crashing down. You have to comply with the ACA, but if one of your employees doesn’t, you’re not at fault in the eyes of the IRS.
4. Learn how it plays into reporting
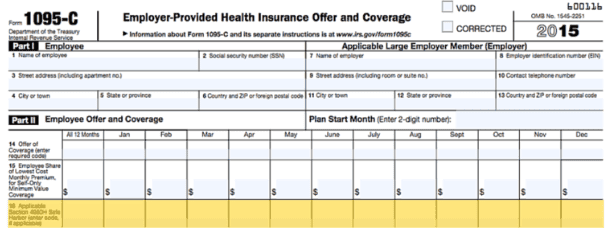
All you have to do is put any code besides 2C on line 16 of your 1095-C form, and that tells the IRS that your teammate waived coverage.
5. You’re done!
Waving goodbye to coverage is just a fact of life for many folks. By studying up on the best course of action, you’ll be able to help your team prepare for all of life’s ebbs and flows.



