
The Patient-Centered Outcomes Research Institute (PCORI) was established by the Affordable Care Act (ACA). PCORI funds research that can help patients and those who care for them make better-informed decisions about their healthcare choices and overall wellness.
The ACA imposes a patient-centered-outcomes-research-trust-fund fee on employers that offer certain types of health insurance policies that are self-insured (also referred to as self-funded) health plans as part of their employee benefits. These fees help fund PCORI and its clinical effectiveness research to improve the quality of health care. In 2019, the Further Consolidated Appropriations Act, 2020 signed into law and extended the PCORI fees through 2029.
This post will explain how PCORI fees may affect your business, what your fee amount might be, and if you are subject to it, how you pay it.
Do I have to pay the PCORI fee?
The ACA requires applicable employers to report and pay the fee once a year, using Form 720 for the Quarterly Federal Excise Tax Return that you can get from IRS.gov. The PCORI fee is due by July 31st. The fee is fixed annually by the Internal Revenue Service (IRS) and adjusted each year for inflation. Employers owe the annual PCORI fee for each eligible employee (aka the average number of lives covered under the policy or plan) covered under the plan.
Health Reimbursement Arrangements (HRAs) like Individual Coverage HRAs (ICHRAs) and Qualified Small Employer HRAs (QSEHRAs) are considered self-insured medical plans for PCORI purposes. Thus, employers who offer these plans owe this fee because plan sponsors of self-insured health plans are subject to the PCORI fee.
The fee applies to policy or plan years ending on or after October 1, 2012, and before October 1, 2029. You can refer to the IRS fee schedule for the filing due date and rates depending upon the month your health plan ended.
What information is needed to fill out IRS Form 720?
To file a Form 720, employers will need to report the average number of lives covered under applicable self-insured health plans. The average number of covered lives is the average number of employees eligible to participate in the plan.
There are three methods an employer can use to calculate the average number of eligible employees. Employers can also choose to use a third-party administrator to handle these calculations for you. Below are the method options used to calculate a company’s total fees based on the guidance from the IRS:
Actual count method: The total number of lives covered for each day of the policy year and dividing that total by the number of days in the policy year.
Snapshot method: The totals of lives covered on a designated date during the first, second, or third month of each quarter (or more dates in each quarter if an equal number of dates is used for each quarter), and dividing that total by the number of designated dates used.
Form 5500 method: Sum of: 1) the total participants identified on Form 5500 at the beginning of the year and 2) the total participants identified on Form 5500 at the end of the year. Divide this sum by 2.
How to file Form 720
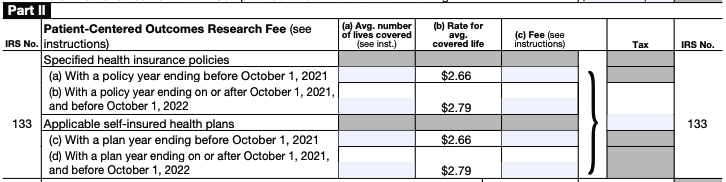
To report and pay the PCORI fee, an employer should first complete Form 720, filling out the PCORI section that can be found on the second page of the form, under Part II, IRS No. 133. This is where an employer will report the average number of participants (i.e., eligible employees) using one of the calculation methods described in the section above.
According to the IRS, if you’re filing the second quarter Form 720 only to report the PCOR fee, then you don’t have to file for other quarters unless you have to report other fees or taxes. Since employers may need to fill out other sections of the form for other business purposes, it’s best to consult with a tax professional before completing and filing 2nd quarter Form 720.
To submit the associated PCORI fee, reference the final page of Form 720, titled the Form 720-V, Payment Voucher. To complete this section, the employer will need their employer identification number (EIN) and include the PCORI fee payment the employer owes the IRS, as calculated in Part II, IRS No. 133.

Employers may need to fill out other sections of the form for other business purposes. It is best to consult with a tax professional before completing and submitting Form 720.
There are two ways to file a completed Form 720: electronically or by mail. An employer can electronically file the completed form through any IRS-approved electronic return provider. The Electronic Federal Tax Payment System (EFTPS) can also be used to pay the fee. Alternatively, employers can mail their completed Form 720 and payment to:
Department of Treasury
Internal Revenue Service
Ogden, UT 84201-0009
What is the PCORI deadline?
The PCORI fee is due July 31st of the calendar year immediately following the last day of the plan year or policy year to which the fee applies.



