
The State of Small Business Health Insurance through the Lens of Gusto Data

The current spending bill in Congress contemplates an historic expansion of social spending to support American workers, families and businesses, as well as make deep investments in long-term economic competitiveness. One of the pillars of worker and family well-being is health insurance, and workers see health insurance as a key benefit when making decisions about where to work. Has the cost and onerousness of providing health insurance to employees deterred smaller employers from offering health insurance, and are current public incentives right-sized to encourage smaller employers to offer this vital benefit to their employees?
Platform data from Gusto—the payroll, benefits, and HR services platform for 200,000+ small-and-medium-sized businesses nationwide—sheds light on the state of small business health insurance and identifies areas for policy action that would increase small employers’ ability to offer health benefits to their employees.
Data Highlights
Firms with 50-99 employees are 5.3x more likely to offer health insurance than firms with 1-9 employees. In general, the likelihood of offering health insurance decreases with firm size.
The smallest businesses contribute approximately two-thirds of what the largest businesses contribute to employees individual and dependent premiums.
Most employees working for Gusto’s customers have incomes that are too high to qualify for existing employer incentives, such as the Small Business Health Options Program (SHOP) Exchange tax credits.
Key Takeaways
Firms with 1-25 employees are the most disadvantaged in providing health insurance. Policy efforts to make health insurance more affordable and accessible to these employers could substantially improve the rate of employer-based coverage. An increase to the income eligibility threshold and decrease to the employer contribution of the Small Business Health Options Program (SHOP) Exchange would enable more small businesses to participate in the program, thus enabling more working Americans health care through their employers.
Smaller employers are a large disadvantage compared to larger employers in their ability to offer health insurance to their employees, which may reduce their competitiveness in attracting and retaining high-quality talent. An expansion of tax credits would enable small businesses to charge employees less for their health insurance premiums, which better aligns with large corporate offerings. Similarly, an increase to the income eligibility threshold and decrease to the employee contribution would enable additional small businesses to participate in the SHOP Exchange.
Income limits and contribution requirements created in the ACA penalize smaller employers in professional sectors for paying competitive rates by disqualifying them from assistance to provide coverage. Tax incentives, subsidies, and other incentives to encourage employers to offer coverage and contribute more can increase the attractiveness of small business employment by top talent, thereby contributing to small employers’ economic competitiveness.
Analysis
Employer Coverage by Business Size
Most small employers (1-49 employees) do not provide health insurance to their workers. Yet, there is large variation among different firm sizes. The smallest firms are the least likely to offer health insurance to their employees, at a rate of 14.4%. Firms with 10-24 employees are 3.3x more likely than smaller firms to offer insurance (48.0%), yet are only 64% as likely as those with 50-99 employees, who are federally mandated to provide health insurance.
Figure 1: Percentage of Employers Who Provide Health Insurance to Their Employees
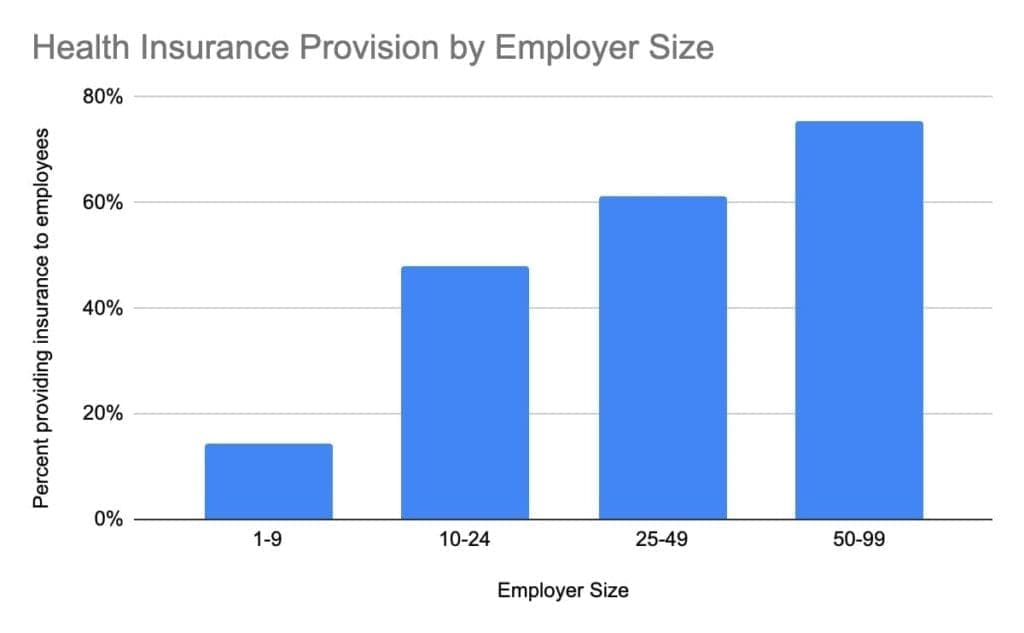
Firms with 1-9 employees have both the lowest coverage and the largest population of employees and offer the largest opportunity to expand coverage. If 75% of firms with 1-9 employees offered health insurance (a 5.2x increase), it would increase the number of insured employees by approximately 650%. Similar gains could be made through policies to increase coverage through employers with 10-24 employees; a 56% increase in coverage among firms with 10-24 employees (75% total coverage rate) would yield a near 300% increase in the number of employees covered through their employer.
Premiums, Contributions, and Deductibles
Table 1: Average and Median Premiums, Deductibles, Out-of-Pocket Costs, and Employer Contributions for Individual Coverage
ER Size | Average Annual Premium | Median Annual Premium | Average ER Contribution | Median ER Contribution | Average Deductible | Median Deductible | Average MOOP | Median MOOP |
1-9 | $6,322 | $5,748 | $3,824 | $3,035 | $2,769 | $2,500 | $6,337 | $6,600 |
10-24 | $6,223 | $5,700 | $4,646 | $4,001 | $2,689 | $2,250 | $6,259 | $6,550 |
25-49 | $6,277 | $5,820 | $5,546 | $4,743 | $2,591 | $2,250 | $6,124 | $6,500 |
50-99 | $6,271 | $5,820 | $5,471 | $4,587 | $2,544 | $2,250 | $6,137 | $6,500 |
100+ | $5,871 | $5,556 | $5,314 | $5,216 | $2,485 | $2,250 | $5,587 | $6,000 |
Individual average and median premiums are between 7-8% costlier for the smallest businesses than the largest in our sample. Though premiums are somewhat comparable, the smaller firms in Gusto’s sample indicate that ERs contribute substantially less to annual premiums than larger businesses do, as shown in Table 2 below.
Table 2: Percentage of Employer Contribution Towards Employee Premiums
ER Size | ER Contribution to Individual Premium | ER Contribution to Dependent Premiums |
1-9 | 60.49% | 36.86% |
10-24 | 74.65% | 42.66% |
25-49 | 95.28% | 51.97% |
50-99 | 94.00% | 59.66% |
100+ | 95.64% | 52.99% |
According to the Kaiser Family Foundation (KFF) data, the 2019 average individual premium in the United States was $6,972, of which the employee paid 21%, and the employer paid 79%. Table 3 indicates that the average in the KFF survey masks large and systematic variation among firm sizes, with the smallest businesses unable to contribute close to this amount.
Table 3: Average and Median Premiums, Deductibles, Out-of-Pocket Costs, and Employer Contributions for Family Coverage
ER Size | Mean Annual Premium | Median Annual Premium | Mean ER Dependent Contribution | Median ER Dependent Contribution | Mean Family Deductible | Median Deductible | Mean Family MOOP | Median Family MOOP |
1-9 | $17,784 | $16,440 | $6,556 | $2,096 | $5,671 | $5,000 | $12,572 | $13,100 |
10-24 | $17,638 | $16,289 | $7,524 | $4,825 | $5,469 | $4,500 | $12,373 | $13,100 |
25-49 | $18,025 | $16,597 | $9,368 | $7,969 | $5,479 | $4,500 | $12,292 | $13,100 |
50-99 | $17,752 | $16,257 | $10,591 | $9,546 | $5,014 | $4,000 | $12,088 | $13,000 |
100+ | $15,337 | $13,641 | $8,127 | $7,219 | $5,026 | $4,000 | $11,284 | $13,000 |
Again, the annual family premium for <100 EE firms is costlier than for larger firms. The average annual family premium for the most expensive group, 10-24 EEs is 17% more expensive than that of 100+ EE firms; the median is 23% more expensive for these same groups. Again, the contribution of smaller ERs to premiums for dependents is significantly lower than that of larger firms, shown in Table 3 above.
The fact that premium costs are comparable across employer size, but contributions vary substantially indicates that smaller employers care about providing a health insurance benefit of similar quality to larger firms, but are unable to contribute the same amounts to cover the costs. Current tax credit programs require that smaller employers contribute at least 50% to cover premiums. The lower contribution level by smaller employers indicates that a substantial portion of smaller businesses are not being served by currently available incentives and support to provide health insurance to their employees.
Employee Income and Tax Credit Eligibility
Figure 2: Estimated Annual Income of Small Business Employees
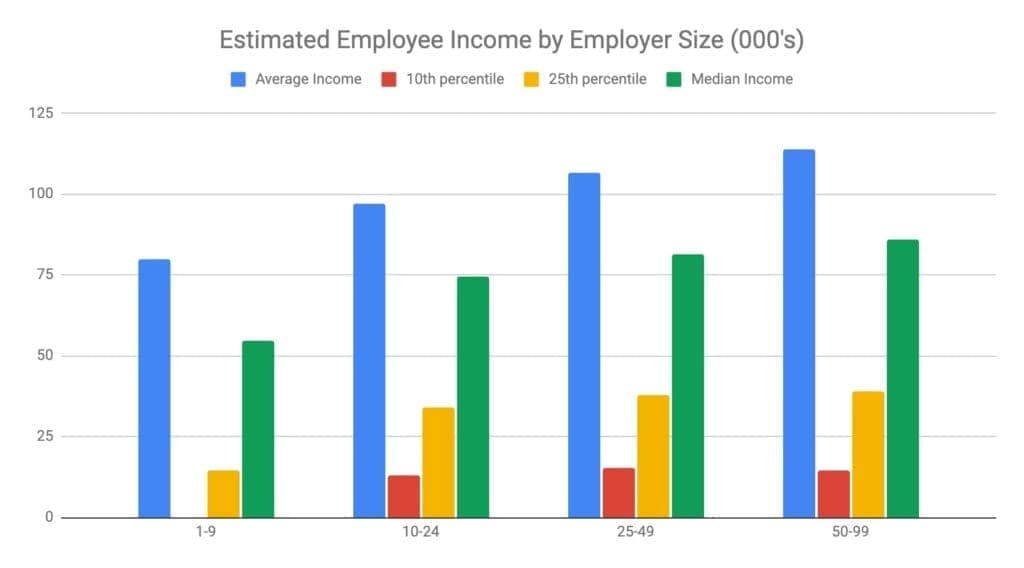
In Gusto’s sample, most employers are not eligible for tax credits due to the income of their employees. Across all size categories, the average employee wage was significantly above the $50,000 average annual income per employee income that is required to receive currently available tax credits.
Conclusion
Health insurance is a critical benefit valued by employees at companies of all sizes. According to the Society for Human Resource Management (SHRM), 46% of workers view health insurance as a positive or deciding factor in their decision to accept a new job; 56% consider it a key aspect of their decision to stay with an employer. Supporting smaller employers to offer health insurance to employees can increase health insurance coverage as well as contribute to the competitiveness of smaller businesses in attracting and retaining key talent.
Methodology
In this post, we use platform data from Gusto – the people platform offering full-service payroll, benefits, compliance, and expert HR services for 200,000+ small-and-medium-sized businesses nationwide. We took a sample of employers and their workers who were active in 2021, and analyzed their data to conduct an analysis of their premiums, rates of coverage, and contributions, across company sizes.
Gusto’s customers skew towards desk-based knowledge and creative industries, although all industrial sectors are represented among Gusto’s more than 200,000 customers. Except where otherwise noted, this analysis is based on information on health insurance purchased through Gusto’s health insurance brokerage service, which currently offers more than 5,000 ACA-compliant, fully insured, small group plans to its customers.



